Introduction
Kawasaki disease (KD) is an acute systemic vasculitic syndrome most common in children [1]. The diagnosis of KD is based mainly on clinical feature (Table 1) and no specific diagnostic test exists. Several studies reported N-terminal pro-brain natriuretic peptide (NT-proBNP) level in patients with the acute phase of KD as a useful marker of diagnosis [2вАУ4].
Table 1.
Diagnostic criteria for Kawasaki disease.
Determining of KD in emergency department (ED) is diagnostic challenge if the duration of febrile days is not clear. The delayed diagnosis of KD in the ED might cause confirmative diagnosis of KD about three, four, or more days, and it can increase the risk of coronary artery aneurysm.
Many studies showed NT-proBNP may help diagnosis KD [2вАУ4]. But, the appropriate level of NT-proBNP for differentiating KD in ED has not yet been suggested. The purpose of this study was to determine whether the serum NT-proBNP level could be a useful marker for patients with the acute phase of KD in ED, especially when febrile duration was less than 5days. And we also planned to evaluate the performance of NT-proBNP in diagnosing KD to estimate the threshold for differentiating KD from other febrile illnesses in ED.
Methods
From January 2011 to December 2012, children aged 1 month to 10 years who presented at ED with symptoms suspected KD with less than five febrile days. They underwent NT-proBNP sampling in ED.
And KD group was defined following classical diagnostic criteria as shown in Table 1. Demographic data, such as the age or sex, and clinical data, such as the day of illness were compared between KD and controls. Patients with less than 5 febrile days were grouped separately in both groups. Patients with uncorrected significant structural heart disease, known cardiomyopathy, septicemia or septic shock, hypovolemic shock, prolonged fever of unknown etiology, renal failure, patients undergoing or who had undergone chemotherapy involving cardiotoxic drugs and a history of confirmed KD were excluded. NT-proBNP levels of KD with less than five days of fever were compared and Receiver Operator Characteristic (ROC) analysis were obtained for determining cutoff value.
Statistical analyses were performed with STATA 13.1 software (Stata Corp LP). Data are expressed either as median; interquartile range for continuous data or median (range) for categorical data. Nonparametric analysis (Mann-Whitney U test) was utilized for continuous data that did not follow a normal distribution. Rank sum test was also used to compare paired data and to compare grades. ROC analysis was performed to define the serum NT-proBNP concentration at which the sensitivity and specificity were optimal. Odds ratios and 95% confidence intervals (95% Confidence Interval, CI) were calculated. Fisher exact test and chi-square test with Yates correction for continuity were used for categorical data distribution.
Results
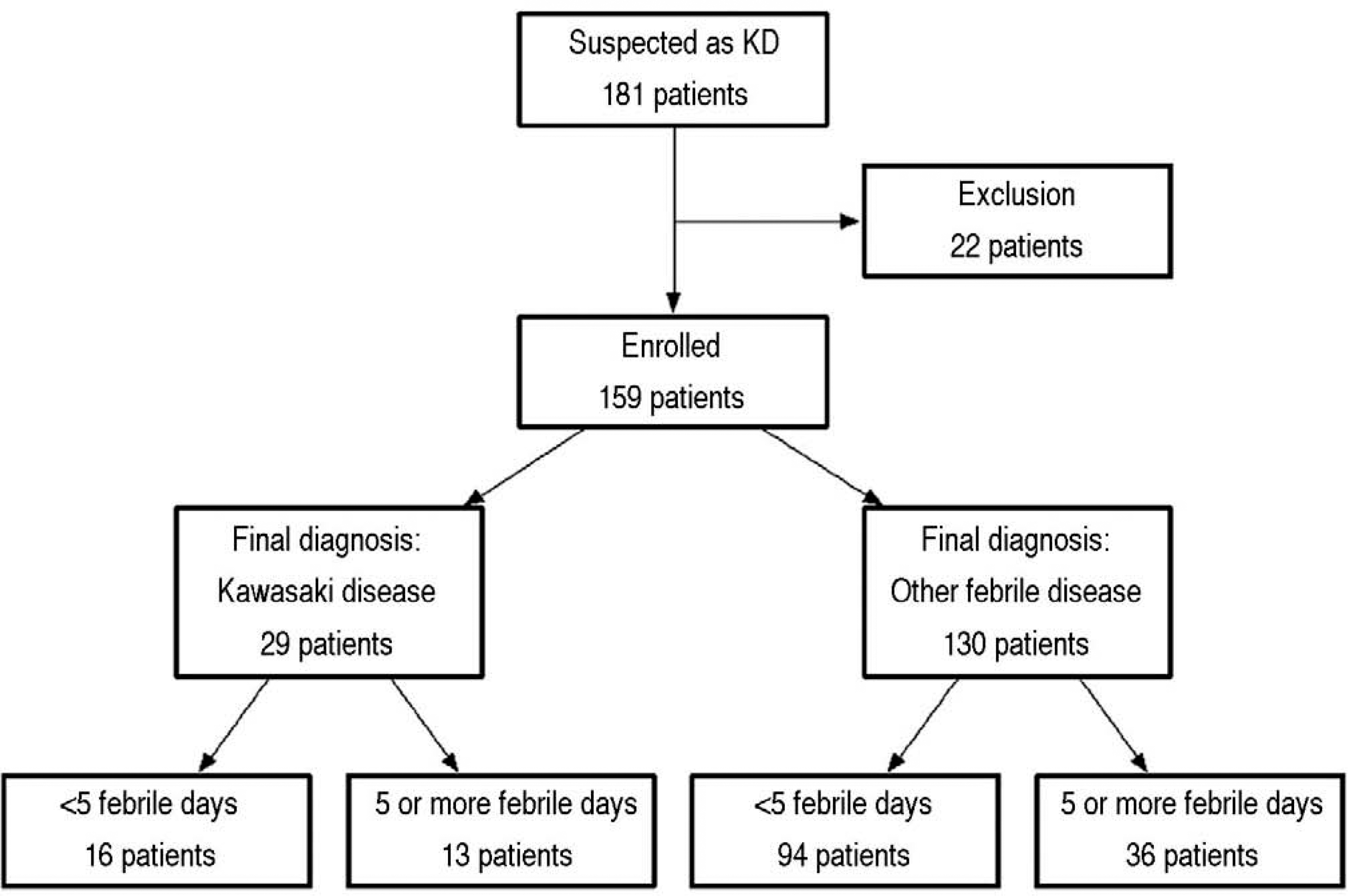
One hundred and eighty one patients were included. Twenty two patients were excluded, 29 patients were eligible for the KD group and 130 patients with other febrile illnesses were enrolled as controls finally (Fig. 1). Sixteen patients in the KD group and 94 patients in the other febrile illness group had less than 4 febrile days when presented at ED. Patients diagnosed with KD at ED or outpatient clinic during the period of follow-up after discharge from ED fulfilled the Criteria for Diagnostic Guideline established by the Kawasaki Disease Research Committee in Japan. Serum NT-proBNP level was measured at least once in all patients at the time of admission to ED.
There was no significant difference in the age, sex and duration of fever between KD and other febrile illness groups (Table 2). There was a higher serum NT-proBNP level in KD group (322.8 [14.9вАУ1579.3] vs 80.0 [6.7вАУ488.9] pg/mL; P=0.01) in comparison with the patients in the other febrile disease group (Table 2).
Table 2.
Demographic characteristics in KD and other febrile illness, in the cases of less than 5 days of fever.
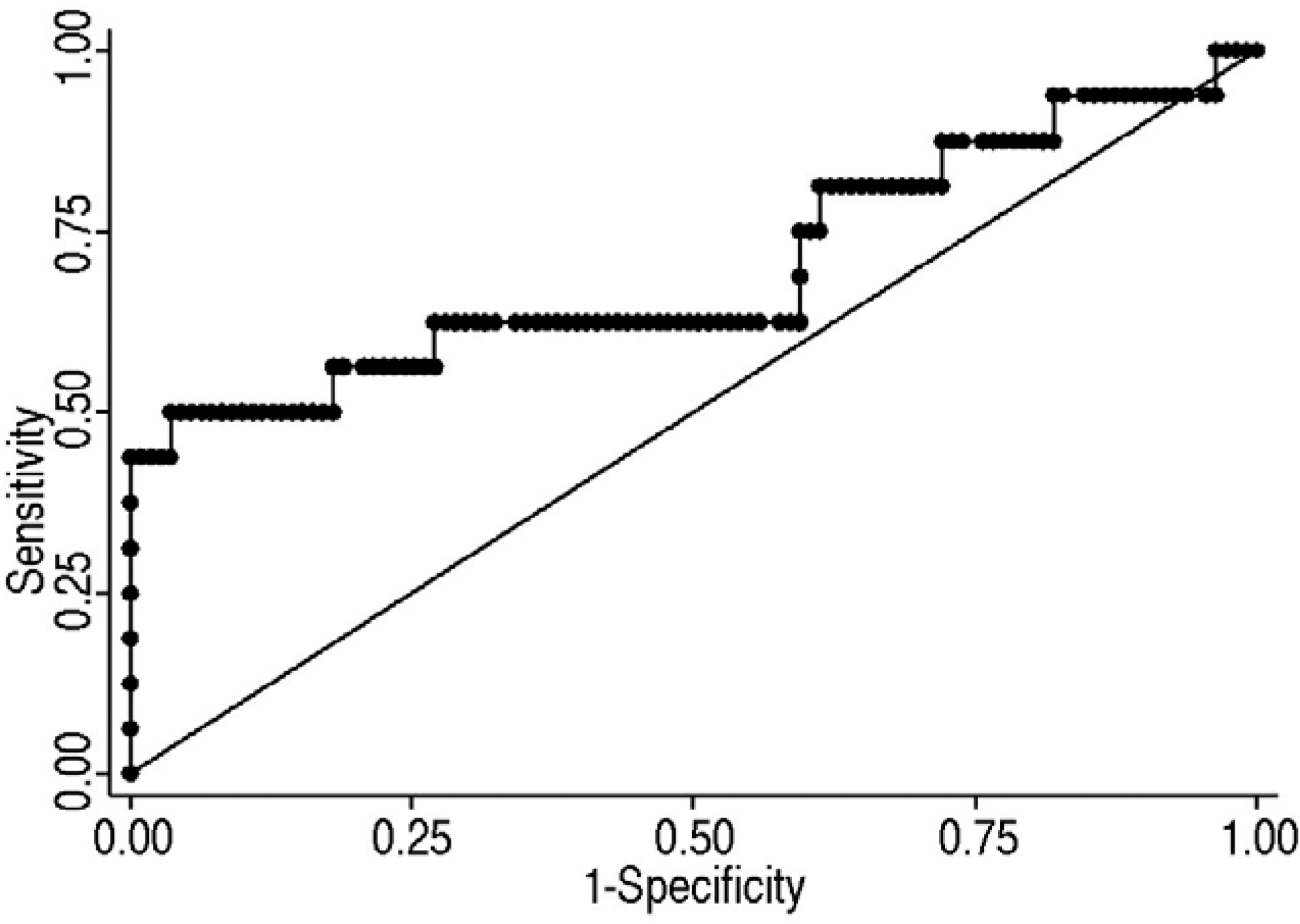
The serum NT-proBNP levels to KD in patients with less than 5 febrile days were assessed by a receiver operating characteristic curves analysis (Fig. 2). A NT-proBNP cut-off value of 105.5 pg/mL yielded a sensitivity of 62.5%, a specificity of 73.0%. The area under the curve of NT-proBNP for predicting KD in less than 5 febrile group was 0.701 (Fig. 2).
Discussion
The results of this study show that serum NT-proBNP may be useful as a clinical marker for diagnosis of acute phase of KD in ED in the case of less than 5 febrile days. The cut-off value of NT-proBNP is 105.5 pg/mL and sensitivity and specificity is 62.5% and 73.0%.
Fever, bilateral non-exudative conjunctivitis, erythema of the lips and oral mucosa, changes in the extremities, polymorphous exanthem, and cervical lymphadenopathy are classical clinical presentation of KD [1,5]. But, these indicators are not all present on any given day in many cases [6]. Some laboratory findings can help in identifying KD: the presence of raised white blood cell count white blood cells in microscopy of urine analysis, and raised transaminases or bilirubin [1,6,7]. However, these tests are neither pathognomonic nor diagnostic. Diagnosis and treatment are delayed to confirm a fever persisting for at least 5 days in patients presenting with incomplete clinical features of KD [2].
There is no report of diagnosis of KD in ED. It seems that diagnosis of KD is more difficult than in clinic especially when duration of fever is less than 5 days or the symptoms are incomplete. KD is associated with the elevation of inflammatory markers including Erythrocyte Sedimentation Ratio (ESR), C-Reactive Protein (CRP) and platelet count [8]. Using the algorithm of the American Heart Association (AHA) for diagnosis of incomplete KD, laboratory tests are recommended when a patient has fever in addition to two or more clinical criteria of KD [9]. Incomplete Kawasaki disease should be considered in all children with unexplained fever for вЙ•5 days associated with 2 or 3 of the principal clinical features of Kawasaki disease. The AHA recommended a diagnostic algorithm of incomplete Kawasaki disease which comprises of 6 supplemental laboratory and echocardiographic criteria (Table 3). Echocardiography and intravenous immunoglobulin administration should be considered when the CRP level is 3 mg/dL or higher or when the ESR is 40 mm/h or faster. But, these laboratory tests can be increased in other febrile diseases in ED and these result can be useless in differentiation of KD from other illness in ED frequently.
Table 3.
Supplemental laboratory criteria (A) and echocardiographic criteria (B) for the diagnosis of incomplete Kawasaki disease prepared by the American Heart Association.
| (A) |
| Serum albumin вЙ§ 3.0g/dL |
| Anemia for age |
| Elevation of alanine aminotransferase |
| Platelet after 7 days вЙ•450,000/mm3 |
| WBC вЙ• 15000/mm3 |
| Urine WBC вЙ• 10/HPF |
| (B) |
| Z score of LAD or RCA вЙ• 2.5 |
| вАГCoronary arteries meet Japanese Ministry of Health criteria for aneurysm 26 |
| вАГInternal lumen diameter: >3 mm in children <5 years old, or >4 mm in children <5 years old |
| вАГOf a segment measures вЙ• 1.5 times that of an adjacent segment |
| вАГClearly irregular coronary lumen |
| Other 6 suggestive features (if вЙ• 3 features, positive) |
| вАГPerivascular brightness of coronary arteries |
| вАГLack of tapering of coronary arteries |
| вАГDecreased LV function |
| вАГMitral regurgitation |
| вАГPericardial effusion |
| вАГZ score in LAD or RCA of 2 to 2.5 |
Several studies reported increased plasma NT-proBNP level in patients with the acute phase of KD thus providing a useful marker for diagnosing KD [2вАУ4,10,11]. Dahdah et al. reported pre-intravenous immunoglobulin NT-proBNP levels were significantly higher in KD patients than in controls (923.6¬±1361.7 vs. 186.2¬±198.0 ng/L; P<0.001) [2]. Cho et al. [3] reported NT-proBNP levels were significantly higher in the KD patients than in the controls (P<0.001). In the ROC curve analysis, the sensitivity was 66.1%, and the specificity was 77.1% at 235.2 pg/mL. NT-proBNP is the best available predictive value according to these studies, unlike the currently used laboratory tests. But there had been no evaluated study about usefulness of NT-proBNP level in ED as an adjuvant laboratory marker of acute phase of KD. A NT-proBNP cutoff value of 105.5 pg/mL yielded a sensitivity of 62.5%, a specificity of 73.0% in this study. Shorter febrile days of this study population might affect the lower value of NT-proBNP compared with other studies.
This study has several limitations. First, this study includes its retrospective nature and the numbers of patients are different in KD and control group. Second, the statistical conclusion might be influenced by the small number of patients with KD and non-parametric statistical tests performed over. Further study will be required for comparison between similar groups. Third limitation may have been related to the variety in the diagnoses of the febrile controls. The categories of febrile diseases should be considered future study.
Conclusion
These findings will doubtless be much scrutinized, but there is a immediately dependable conclusion that NT-proBNP can be an adjuvant laboratory marker for KD in ED if the fever duration is less than 5 days. A prospective multicenter study with emphasis on NT-proBNP in a diagnostic algorithm of KD in ED is needed.